
In recent weeks, through midwifery meetings, webinars, or films, I’ve been exposed to some new and interesting things. Here are a few of them to share and think about! I’ve been working hard on the 2nd draft of my upcoming book Confessions of a Childbirth Educator, so I’m taking advantage of the blog to not have to use citations!
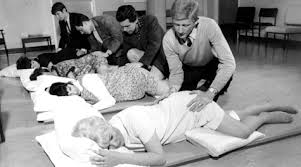
LAMAZE HISTORY
The origins of Lamaze (associated in the Western world as “breathing techniques”) began in the Soviet Union, but are widely unrecognized. In the 1940s-1950s, based on Ivan Pavlov’s research, Soviet obstetricians developed what they called “psychoprophylaxis” for childbirth. The idea was that conditioning and conditioned reflexes could reduce pain. The “new Soviet woman” of the socialist republic would be rigorously trained, as if for an athletic competition. During pregnancy, groups of women partook in a regimen of exercise, leisure, and community, with the goal of a painless, arguably almost “superwoman,” childbirth. The state-supported training involved concentration, focus, using particular muscles, discipline, and control, including breath control. Training “camps” were literally created, with disciplined routines, that also included group fun and leisure time, to create the “optimal” birthing woman, who would give birth without anesthesia.
Dr. Ferdinand Lamaze visited the USSR from France in 1951, was impressed by the methods, and brought them back to France, where they spread across Europe, and eventually to the U.S.
At first, when widely popularized in the 1970s, the “Lamaze method” was actually a rebellion against the traditional view that doctors should be in charge of everything. It represented Active vs. Passive participation in the birth, as well as including husbands in the process. Feminism, which had advocated anesthesia for “painless childbirth” as a source of empowerment in the earlier decades, switched to a creed of empowering one’s self through involvement and agency in the birth experience.
PRESENT DAY ISSUES
The midwives and doulas discussed why labors seem to be going slower in recent years. They are seeing more frequent stalled labors and delayed progress. One of the possible explanations raised was that women potentially have less oxytocin than in the past; they are “oxytocin-deprived.” Why? Less connection with others – working from home, cell phones, computers, technology (prior, also covid) all lead to more isolation. Oxytocin thrives on bonding, emotional connection, trust, and attachment.
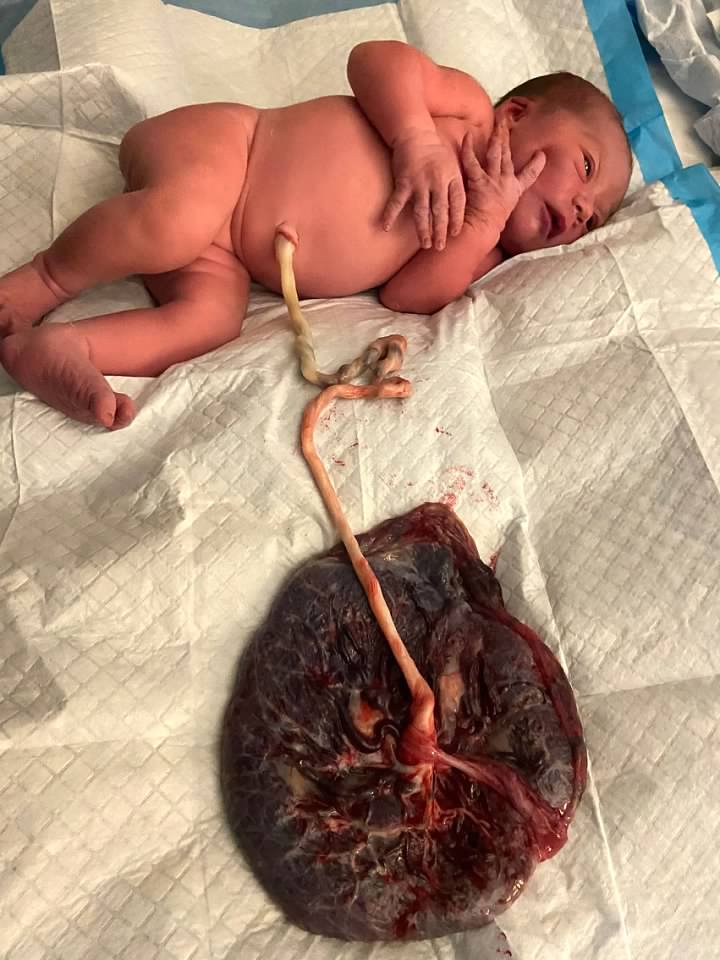
PLACENTA
Experiments (both anecdotal & research; lots more research is needed) are showing the huge reparative qualities of the chorion, amnion, and umbilical cord (chorion and amnion are the membranes surrounding the baby, forming the amniotic sac which holds the fluid, ie. “bag of waters”). Amazing discoveries (possibly known by midwives for centuries) are revealing beneficial usage of these parts for skin grafting, artery grafting, and healing of wounds. One well-known midwife has found that slicing the cord and putting pieces onto wounds, especially the Whartons Jelly that surrounds the cord, has almost immediate restorative healing properties. Putting a piece of placenta and cord under the tongue is seen to stop a hemmorhage.
The “direct experience” of multiple midwives should be viewed as “evidence.”
Technology is being developed for creating artificial placentas, to increase survival rates for preterm infants.
*** There are many products being made from women’s placentas (and cords) but women are not being compensated. It is the only body organ that is taken without permission and used for profit. The hospitals sell the placentas to these manufacturers. Hospitals should have to get permission to sell your placenta.
EARLY RUPTURE OF MEMBRANES
Midwives have seen membranes rupture before 37 weeks and have found several things to be true. It could be just a “fluke,” resulting in 3 or 4 days ruptured and then a fast labor. It could be from a pre-existing infection (rather than an infection that is commonly viewed as brought on by the rupture), in which case, when it is prior to 37 weeks and we want to keep the baby in as long as possible, antibiotics (ampicillin) can be given.
ELECTIVE C-SECTIONS
The average worldwide rate of MRCB (mother-requested cesarean birth) is 3%.
The issues that are considered by both mothers and care providers include:
–Tokophobia (extreme phobia of childbirth/pregnancy).
-Worries about: incontinence, perineal damage/tears, pelvic organ prolapse, sexual dysfunction.
-Autonomy (mother-led choice)
-Liability
The World Health Organization still recommends a worldwide cesarean rate of 10-15%. This includes ALL reasons: life-threatening emergencies, complications developed in labor (fetal distress, lack of progress), repeat cesareans, and MRCB.
IV
IV fluids in large amounts can result in Fluid Overload. Complications include:
-Dilution of the mom’s blood clotting (dangerous if hemmorhaging occurs)
-Leakage into the baby’s lungs, causing breathing problems.
-Artificial inflation of birth weight, which can lead to a false diagnosis of inadequate breastfeeding.
